Site Under Development, Content Population and SEO, Soft Launch 1st January 2020
A patient undergoing surgery under anesthesia is usually experiencing a number of disturbances with regard to the normal functioning of several body systems. This means that the patient’s physiological status needsto be monitored at all times. The types of monitoring required vary with the procedure being undertaken.
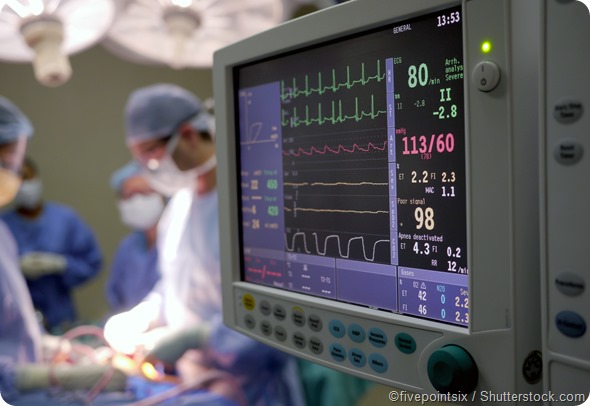
The equipment used to monitor a patient throughout a surgical operation is usually made up of one single system that can be set to accurately and continuously measure a set of patient parameters that reflect the functioning of the body systems. Various sensors and electrodes are attached to the patient to gather information. These measurements are displayed on monitors.
The parameters measured in most surgical procedures include:
The core body temperature is tightly controlled in humans, because all body tissues function optimally within a narrow range of temperature. This is usually 2 to 4 degrees warmer[?]than the skin temperature over the limbs, which depends on many other factors such as the ambient heat exposure, and vasoconstriction.
When surgical operations are performed, the patient is typically exposed to a cold environment, as well as dilution of the warm body fluids by colder intravenous infusions. The surgical incision also contributes to heat loss from the body via evaporation of various fluids from the opening. However, this alone is insufficient to induce hypothermia in a normal patient. Instead, the normal process of thermoregulation drives up the body heat production to maintain an even temperature.
Anesthesia can cause hypothermiaif the surgical patient is not monitored carefully. Core temperature may be directly measured at sites such as the distal esophagus, the pulmonary artery, or the ear drum (tympanic membrane). However, other sites which indicate a consistent relationship with the core temperature are generally used for clinical purposes, such as the bladder, rectum, or even the axilla.
Hypothermia has consistently been shown to worsen the postoperative course of the patient, inducing complications such as:
A general anesthetic shuts down many brain functions temporarily, including the temperature regulating centers. This results in a significant depression of core temperature, and threatened hypothermia. This triggers immediate compensatory reactions such as shivering and vasoconstriction. Shivering is a rapid contraction of the skeletal muscles which induces combustion of fuel and energy expenditure to produce heat. Vasoconstriction shunts blood from the peripheral circulation to the deeper organs, preserving the heat distribution to vital functions.
Spinal anesthesia can also cause hypothermia, but the fall in core temperature may not be as marked as that following the use of a general anesthetic. These patients are unable to sense the hypothermia as a result of autonomic impairment, coupled with failure of regulatory mechanisms. Temperature measurement during the surgical procedure is therefore mandatory, coupled with active warming as required.
On the other hand, epidural anesthesia produces hyperthermia of unknown cause.
Thermistors, thermocouples, and infrared thermometers, are the generally used temperature measuring devices that help to detect near-core temperatures within 0.5 degrees.
Circulatory impairment may occur during the intraoperative period, as a result of the change in cardiac contractility, oxygenation, and hypotension. This may persist after the procedure, and trigger a cascade of inflammatory cytokines, which is responsible for multi-organ dysfunction. Monitoring for this complication includes arterial pressure monitoring, urine output, arterial pH monitoring, and blood lactate. Generalized tissue hypoxia is often persistent despite normalization of cardiovascular parameters, and therefore invasive monitoring is warranted in high-risk or critical patients.
Arterial oxygen saturation is measured non-invasively by infrared oximeters which are based on the principle of reflection spectrophotometers. Light is directed into the bloodstream, and it reflects off the blood cells. The reflected blood is read by a photodetection device.
Invasive monitoring of oxygen saturation is by a pulmonary artery catheter which measures mixed venous oxygen saturation, while the oxygen saturation in the central veins is measured by a central venous catheter.
Intraoperative neurophysiological monitoring is used when surgery involves the central or peripheral nervous system, and helps detect changes in the integrity or function of the nervous structures in and near the operative field, or those which could be affected by the surgery. Some examples include monitoring of the recurrent laryngeal nerve during thyroid surgery, the facial nerve during facial surgery, and the brainstem during surgery on the cerebellopontine angle.
Electrical potentials created by nerve cells upon stimulation, both spontaneous and evoked, are recorded and studied to assess their normalcy or otherwise. The technique is effective in preventing neurologic injury following surgery on anatomical structures that could potentially impact nervous system functioning and health.